Member organizations that participate in an Employers Health PBM program enjoy an uncommon feature known as an annual “Market Check.” What is the Market Check and what role does it play in delivering value to plan sponsors?
Customary PBM Contracts
The pharmaceutical marketplace is dynamic. However, most agreements between PBMs and pharmacy benefit plan sponsors are not.
The pricing incorporated into a PBM agreement is based on a risk-adjusted projection of the discount levels the PBM believes it can achieve over the contract term. In other words, the pricing is based on the discounts the PBM thinks it can get. And, in general, direct agreements between PBMs and pharmacy benefit plan sponsors have a minimum three-year term, and the pricing is established before the term begins.
Groups currently participating in the last year of a three-year PBM agreement more than likely negotiated pricing terms in 2012. A lot has happened since then. PBM consolidation, exclusionary formulary strategies, increasing specialty utilization, changing brand drug pricing strategies, AWP inflation, and stabilizing generic dispensing rates are some of the market dynamics that have had an impact on pharmacy benefit costs over the past several years. PBM deals struck in 2012 may or may not have appropriately captured the financial impact of these market dynamics.
Multiyear PBM arrangements reduce administrative burden, but they often fail to consider emerging market dynamics over the course of the contract. As a result, the pricing in multiyear PBM arrangements often grows stale in the second or third contract year. Employers Health avoids this problem by engaging in an uncommon annual process known as a Market Check. Through this process, and pursuant to agreement with its PBM suppliers, Employers Health annually renegotiates the pricing available to groups participating in Employers Health PBM programs.
Saving Time and Money through the Employers Health Annual Market Check
The Employers Health Market Check process is conducted in a manner that, to the extent possible, simulates a full PBM vendor selection process. At the end of each calendar year, Employers Health compares its pricing with 10 or more comparable PBM programs administered by multiple PBMs, then analyzes the results. This competitive analysis and the leverage that comes from nearly $1 billion in annual drug spend enables Employers Health to adjust the pricing terms offered to its participating groups in a manner that capitalizes on market dynamics.
The table below shows the year-over-year pricing improvements (as a percent of total drug spend) Employers Health has been able to secure for its participating groups through the Market Check process.
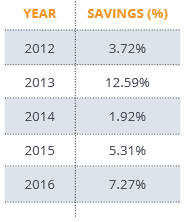
With the Market Check improvements for 2016, Employers Health’s PBM program pricing for 2016 is projected to be between 3 percent and 16 percent more competitive than the market, depending upon group size. Without annual Market Check improvements, Employers Health’s PBM program pricing would still be competitive, but not nearly as competitive as it is with the Market Check improvements.
Conducting an annual Market check is a critical process that must be executed to maintain the most competitive pricing possible. But most pharmacy benefit plan sponsors lack the time, staff or leverage to evaluate their PBM program on an annual basis. That is why employers Health and its expert staff do the work necessary to ensure that the PBM pricing afforded to its members never grows stale and is always among the most competitive in the market.
Download Insight

